teaser
Steven Solga
MD
E:[email protected]
Anna Mae Diehl
MD
Department of Gastroenterology
Johns Hopkins University
School of Medicine
Baltimore, MD
USA
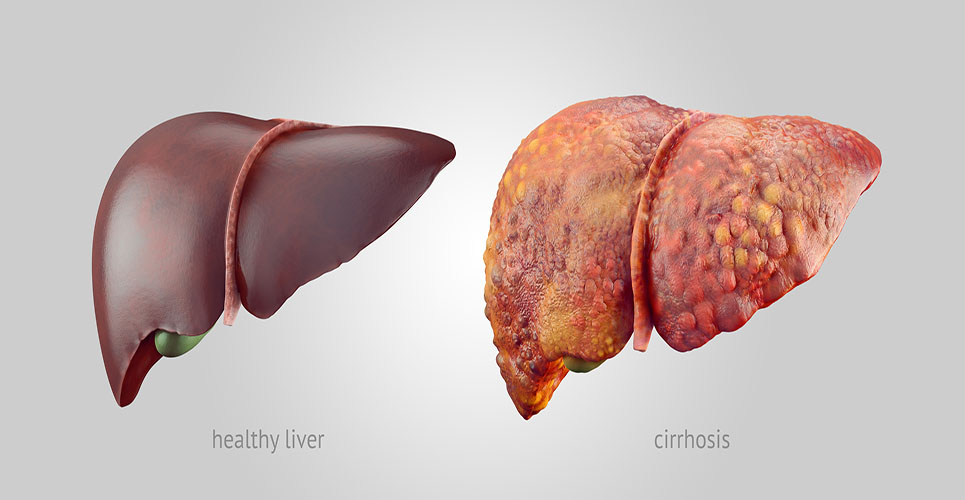
Nonalcoholic fatty liver disease (NAFLD) is a serious and common disease with histological features similar to those of alcoholic fatty liver disease (AFLD). NAFLD includes a broad spectrum of hepatic pathologies, ranging from fatty liver (steatosis) at the most clinically indolent extreme to cirrhosis at the opposite extreme, where most liver-specific morbidity and mortality occurs.(1) Although steatosis is frequently clinically silent, this lesion predisposes the liver to serious damage by additional insults, such as exposure to lipopolysaccharide (LPS), certain hepatotoxins or infectious agents, leading to the eventual development of cirrhosis.(2) Nonalcoholic steatohepatitis (NASH) probably represents an intermediate stage, characterised by steatosis with lobular inflammation.
It is important to find a treatment for NAFLD because:
- It is a highly prevalent disease.
- It can cause cirrhosis and death.
- Its incidence is rising.
- It can coexist with and complicate the management and natural history of other liver diseases.
NAFLD is highly prevalent
NAFLD is perhaps the most common disorder of the liver. Analysis of the third National Health and Nutritional Evaluation Survey (NHANES III), conducted in the USA, suggests that 10–24% of American adults have NAFLD,(3) making NAFLD 3-fold more common than diabetes mellitus and 5–10-fold more common than chronic hepatitis C. Other large, population-based surveys in Europe and Japan are in agreement with the US study regarding the high prevalence of this disorder.(4,5)
NAFLD can cause cirrhosis and death
NASH progresses to clinically significant cirrhosis in a small but critical number of individuals.(6) Indeed, NAFLD is now thought to be responsible for most of what was once classified as “cryptogenic” cirrhosis.(7) This type of cirrhosis accounts for half of the annual liver-related deaths and is a major indication for transplantation worldwide.
Unfortunately, NAFLD often recurs after transplantation (even in the absence of known risk factors)(8) and can cause serious morbidity and the need for retransplantation. Donor livers with hepatic steatosis from otherwise “healthy” donors often perform poorly when transplanted, which further complicates matters and makes hepatic steatosis a major cause for rejecting organs for transplantation.(9) Independent predictors of advanced disease appear to include the severity of obesity, diabetes, hyperlipidaemia and increasing age.(10)
The incidence of NAFLD is rising
Major risk factors for NAFLD include obesity, type 2 diabetes, hyperlipidaemia and hypertension (the components of the “metabolic syndrome”); additional minor risk factors are numerous.(11)
Obesity(12,13) and diabetes(14) are increasing in epidemic proportions in Europe and the USA. NAFLD will thus remain an important issue in hepatology in the years to come.
NAFLD and other liver diseases
“Presumed NAFLD” is usually diagnosed only once a clinician has excluded significant alcohol intake and other numerous common liver diseases, such as hepatitis B and C. While such strict exclusions are often necessary for research purposes, NAFLD may coexist with and complicate other liver diseases.(15) For example, there is a growing appreciation that the presence and degree of steatosis on biopsy in patients with hepatitis C is an independent risk factor for poor outcome, including the worsening of fibrosis(16) and hepatocellular cancer.(17)
Pathophysiology
Despite extensive research, the precise mechanisms that cause NAFLD remain elusive. In most cases, multiple “hits” are required, causing fat accumulation, cell injury and inflammation, and ultimately fibrosis and cirrhosis. Insulin resistance, oxidative stress, mitochondrial dysfunction and free fatty acid toxicity are among the causative factors of stress that result in this pathway.
Treatments
Current treatments for NAFLD are based on the understanding of the pathophysiological mechanisms and associated conditions. Due to the critical importance of insulin resistance in NAFLD, for example, medications that improve insulin sensitivity or treat obesity are logical choices as putative NAFLD treatments. To date, however, all such possible NAFLD treatments (medicinal or otherwise) have been evaluated only in small, and frequently uncontrolled, single-centre trials. In many cases, results have been published as abstracts rather than articles. Furthermore, serum “liver function tests” (eg, aminotransferase levels) have often been used as the primary outcome measurement, despite their known poor correlation with histology and disease outcome. Finally, despite the need for safe and effective NAFLD treatments, it must be appreciated that appropriate trials are difficult to conduct: ideally, serial liver biopsies must be evaluated over long periods of time to confidently demonstrate the histological improvement that may translate into clinically meaningful outcomes. While these are common obstacles in hepatology, other liver diseases (eg, hepatitis C) are more easily quantifiable, with intermediate outcome measurements (eg, serum viral clearance) being carried out. All current treatment recommendations must consider these limitations.
Strategies for NAFLD treatment include:
- “Lifestyle” interventions (diet and exercise).
- Improved insulin sensitivity and glycaemic control (thiazolidinediones or metformin).
- Improved lipid control (gemfibrozil).
- Antioxidants (vitamin E).
- Cytoprotective agents (UDCA).
- Other possibilities (alterations in gut flora with probiotics).
“Lifestyle” interventions
Several studies have evaluated the impact of diet and exercise (usually combined) on serum liver function tests and, less frequently, on liver histology. Unfortunately, due to great variations in study design, diet composition and amount of weight lost, it is difficult to draw conclusions from these studies. Andersen and colleagues prospectively evaluated the effect of a formula diet on 41 obese patients with NAFLD.(18) Study subjects underwent liver biopsy before and after a median weight loss of 34kg over a median of 261 days. These authors reported significant improvement in steatosis on rebiopsy, but also a significant worsening of portal inflammation and a trend towards worsening of fibrosis. Recently, Kugelmas and colleagues found that low-fat diet and exercise were associated with improved liver enzymes, cholesterol and plasma hyaluronic acid levels.(19)
Improved insulin sensitivity and glycaemic control
Agents improving insulin sensitivity and glycaemic control are the focus of increasing interest in the treatment of NAFLD, due to several possible beneficial mechanisms of action. Thiazolidinediones, for example, improve skeletal muscle glucose uptake, decrease central adiposity and activate peroxisome proliferator-activated receptor (PPAR)gamma nuclear transcription factor, among other mechanisms.(20) Before its withdrawal from general use, troglitazone had demonstrated promise in improving enzymes and histology.(21) Pioglitazone(22) and rosiglitazone(23) have now demonstrated similar efficacy with improved safety profiles.
Finally, metformin, which first attracted attention in animal models of NAFLD,(24) may also have a role in humans, as indicated by a limited study. Insulin-sensitising agents will probably have a significant impact on the treatment of NAFLD in the future.
Improved lipid control
Gemfibrozil(25) improves liver enzymes, and bezafibrate(26) improves tamoxifen-associated steatohepatitis. Although 3-hydroxy-3-methylglutaryl-co-enzyme A (HMG-CoA) reductase inhibitors may improve liver enzymes and histology in some patients, the potential to cause mitochondrial injury is cause for concern.
Patients with lipid abnormalities and NAFLD should receive appropriate lipid-lowering therapy, but there is less enthusiasm for the use of these agents in NAFLD patients with normal lipid parameters.
Antioxidants
Since most models of the pathogenesis of NAFLD incorporate some degree of oxidative stress, vitamin E, S-adenosyl- methionine, betaine and various combinations of antioxidants have considerable potential in the treatment of NAFLD. Their low cost, tolerability, excellent safety profile and acceptance by the public add to their appeal. Small studies in adults(27) and children(28) have demonstrated improvement in liver enzymes with vitamin E, while betaine improves liver histology.(29)
Cytoprotective agents
Ursodeoxycholic acid (UDCA), a nonhepatotoxic isomer of chenodeoxycholic acid, has been used in multiple cholestatic liver diseases. Despite widespread and long-standing use, it remains unclear whether the beneficial effects of UDCA are primarily mediated through its cytoprotective properties, through immunologic or membrane-stabilising effects, or through a combination of these. At least three pilot trials of UDCA in NAFLD demonstrated improvement in liver enzymes levels.(30–32) However, a recent, larger, multicentre controlled trial did not demonstrate efficacy (the final results are not yet published). Therefore, despite the apparent safety of UDCA, its cost probably cannot be justified.
Other possibilities
As evidence suggests that pathogenic gut flora may have a role in the pathogenesis of NAFLD, therapeutic alterations with antibiotics or probiotics may be beneficial.(33) This hypothesis, however, has not yet been fully demonstrated in humans.
Conclusion
Despite considerable progress in the understanding of the epidemiology and causes of NAFLD, treatment options continue to evolve. Considering that the incidence of this highly prevalent disorder continues to rise, defining an optimal treatment will remain a priority in hepatology in the years to come.
References
- Matteoni CA, et al. Gastroenterology 1999;116:1413-9.
- Diehl AM. Immunol Rev 2000;174:160-71.
- Clark JM, et al. Am J Gastroenterol 2003;98:960-7.
- Nomura H, et al. Jpn J Med 1988;27:142-9.
- Bellentani S, et al. Ann Intern Med 2000;132:112-7.
- Reid AE. Gastroenterology 2001;121:710-23.
- Caldwell SH, et al. Hepatology 1999;29:664-9.
- Poordad F, et al. Am J Transplant 2003;3:1413-7.
- Imber CJ, et al. Liver Transpl 2002;8:415-23.
- Dixon JB, et al. Gastroenterology 2001;121:91-100.
- Neuschwander-Tetri BA, Caldwell SH. Hepatology 2003;37;1202-19.
- Wyatt HR. Prim Care 2003;30:267-79.
- Campbell I. Heart 2003;89 Suppl 2:ii22-4.
- Fisher M. Heart 2003;89 Suppl 2:28-30.
- Clouston AD, Powell EE. Best Prac Res Clin Gastroenterol 2002;16:767-81.
- Castera L, et al. Gut 2003;52:288-92.
- Ohata K, et al. Cancer 2003;97:3036-43.
- Andersen T, et al. J Hepatol 1991;12:224-9.
- Kugelmas M, et al. Hepatology 2003;38:413-9.
- Neuschwander-Tetri BA, Caldwell SH. Hepatology 2003;37:1202-19.
- Caldwell SH, et al. Am J Gastroenterol 2001;96:519-25.
- Azuma T, et al. Hepatology 2002;36:406A.
- Neuschwander-Tetri BA, et al. Hepatology 2002;36:379A.
- Lin HZ, et al. Nat Med 2000;6:998-1003.
- Basaranoglu M, et al. J Hepatol 1999;31:384.
- Saibara T, et al. Lancet 1999;353:1802.
- Hasegawa T, et al. Aliment Pharmacol Ther 2001;15:1667-72.
- Lavine JE. J Pediatr 2000;136:734-8.
- Abdelmalek MF, et al. Am J Gastroenterol 2001;96:2711-7.
- Laurin J, et al. Hepatology 1996;23:1464-7.
- Guma C, et al. Hepatology 1997;26:387A.
- Ceriani R, et al. Hepatology 1998;28:386A.
- Solga SF, Diehl AM. J Hepatol 2003;38:681-7.
Resource
Practice guidelines of the American Association of Liver Diseases (AASLD)
W:www.aasld.org
Event
European Association for the Study of the Liver (EASL)
39th Annual Meeting
Berlin, Germany
14–18 April 2004
W:www.easl.ch