teaser
Pieternel Timmermans
Hospital Pharmacist
Laurentius Hospital
Roermond
The Netherlands
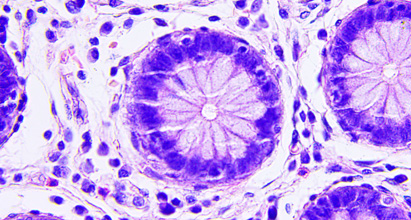
Despite a decrease in the incidence of, and mortality due to, colorectal cancer, this disease is still the second leading cause of cancer-related deaths in Western countries, and the third most common cancer overall. The term colorectal cancer includes cancers of both the large intestine (colon) and the rectum. Most colorectal cancers begin as small, benign clumps of cells (adenomatous polyps), which, over time, might become cancerous.
In advanced colorectal cancers, cancer cells, which have developed in the large bowel, spread outside the bowel or to another part of the body, the most common parts of the body for colorectal cancers to spread being the liver and the lungs. Surgery and adjuvant chemotherapy cannot prevent the frequent recurrence of colorectal cancer, and palliative treatments, which retard the progression of the disease and improve survival rates (from 6–9 months to 15–18 months), have been developed.(1)
In chemotherapy of colorectal cancer, the use of 5-FU and leucovorin (LV), or folinic acid, is still considered the gold standard. New treatments for the management of advanced colorectal cancer include oxaliplatin, which was recently approved by the US Food and Drug Administration, and epidermal growth factor receptor (EGFR)-targeted monoclonal antibody inhibitors. The focus of this article, however, will be on how the standard palliative treatment of advanced colorectal cancer has evolved in the past few years, from chemotherapy in addition to two drugs, 5-FU and LV, to more effective and less toxic ways of administering these drugs (de Gramont regimen) and the association of 5-FU and leucovorin with a new drug, irinotecan (Saltz regimen), which both prolong patient survival.
Mechanism of action
Folinic acid is a derivative of folic acid that is most commonly used as the calcium salt, LV calcium, LV being a mixture of the diastereoisomers of the 5-formyl derivative of tetrahydrofolic acid. The active form of folic acid, which functions as an enzyme cosubstrate, is essential for growth and cellular division, and is required for purine and pyrimidine biosynthesis and the metabolism of amino acids and nucleotides.
The blocking of thymidylate synthetase, a key enzyme in DNA synthesis, has often been used as a target for cancer therapy. 5-FU is a fluorinated pyrimidine antimetabolite that undergoes anabolic and catabolic reactions in the same way as uracil, except that it is converted to thymidine. 5-FU blocks the methylation reaction of deoxyuridylic acid to thymidylic acid and interferes with DNA synthesis. In the presence of 5,10-methylenetetrahydrofolate, 5-fluorodeoxyuridine monophosphate irreversibly binds to thymidylate synthetase.
Indeed, the combination of 5-FU and LV is superior to 5-FU alone for the chemotherapeutic treatment of colorectal cancer, as folinic acid potentiates the antitumour activity of 5-FU.(2)
Treatment regimens
The standard treatment for trying to prevent the spread of colorectal cancer or treat the cancer if it has already spread is chemotherapy associated with 5-FU and LV. The drugs are usually administered together as an intravenous (IV) injection over a few minutes. However, although this regimen is helpful for some patients, many do not benefit and alternative modes of administration have been sought.
The de Gramont regimen
A more effective and less toxic way of administering these drugs was devised in the late 1990s.(3) A multicentre, randomised study on 448 patients with advanced colorectal cancer compared the therapeutic ratio of a monthly schedule of IV low-dose LV (20mg/m(2)) and 5-FU bolus (425mg/m(2)) for 5 days every 4 weeks (the NCCTG–Mayo Clinic regimen) with a bimonthly schedule of IV high-dose LV (200mg/m(2)) as a 2-h infusion followed by bolus 5-FU (400mg/m(2)) and 22-h infusion of 5-FU (600mg/m(2)) for 2 consecutive days every 2 weeks. Results of the study showed that the bimonthly regimen was more effective and less toxic than the monthly one, with more than twice as many patients on this regimen experiencing major tumour shrinkage with fewer side-effects. Therapeutic ratio was also increased with the bimonthly regimen. Unfortunately, there was no evidence of increased survival.
These promising initial results led to a phase II trial of a simplified bimonthly high-dose LV/5-FU regimen consisting of LV (500mg/m(2)/day) and a 48-h continuous infusion of 5-FU (1.5–2g/m(2)/day), administered alone or in combination.(4) This study further showed that high doses of both LV and 5-FU given as continuous infusion improved response rates with acceptable toxicity.
The Saltz regimen
More recently, another regimen, known as the Saltz regimen or triple therapy, has been developed.(5,6) It was known that irinotecan prolonged survival in patients with colorectal cancer refractory to treatment with LV and 5-FU. In a multicentre trial, Saltz and colleagues compared a combination of irinotecan (125mg/m(2) IV), 5-FU (500mg/m(2) as IV bolus) and LV (20mg/m(2) as IV bolus) for 4 weeks every 6 weeks with bolus doses of 5-FU (425mg/m(2)) and LV (20mg/m(2)) daily for 5 consecutive days every 4 weeks as first-line therapy for metastatic colorectal cancer. In a third group, patients were given irinotecan alone (125mg/m(2) IV). Results showed that 5-FU/LV plus irinotecan was superior to 5-FU/LV or irinotecan alone in terms of progression-free survival and overall survival, with patients more likely to have tumour shrinkage and live more than 2 months longer.
Different formulations
We at the Laurentis Hospital (the Netherlands) have started to use a new formulation for folinic acid, consisting of the disodium salt of LV (VoriNa). Unlike the calcium salt, it can easily be mixed with 5-FU in one pump without the risk of crystallisation, which causes catheter obstruction.(7)
A multicentre, phase II study was carried out on 51 patients with metastatic colorectal cancer.(7) A weekly continuous 24-h infusion therapy with 5-FU (2.6g/m2) and simultaneous sodium folinic acid (500mg/m2) dissolved in one pump was administered as first-line therapy for 6 weeks. The treatment cycle was repeated after a 2-week rest period. Results of this study showed that, in the same way as the usual combination 24-h 5-FU plus calcium LV, the combination with sodium folinic acid induced 37.2% objective responses with moderate toxicity. However, tumour progression seemed favourable. In addition, administration of sodium folinic acid is convenient and is cost- and time-saving for the patient in outpatient units.
References
- Nolte W, Ramadori G. Med Klin 2001;96:521-8.
- Milano G, Renee N. Bull Cancer 1995;82:189-95.
- de Gramont A, Bosset JF, Milan C, et al. J Clin Oncol 1997;15:808-15.
- de Gramont A, Louvet C, Andre T, et al. Eur J Cancer 1998;34:619-26.
- Saltz LB, Cox JV, Blanke C, et al. N Engl J Med 2000;343:905-14.
- Benson AB IIIrd, Goldberg RM. Semin Oncol 2003;30 Suppl 6:68-77.
- Hartung G, Hofheinz RD, Wein A, et al. Onkologie 2001;24:457-62.