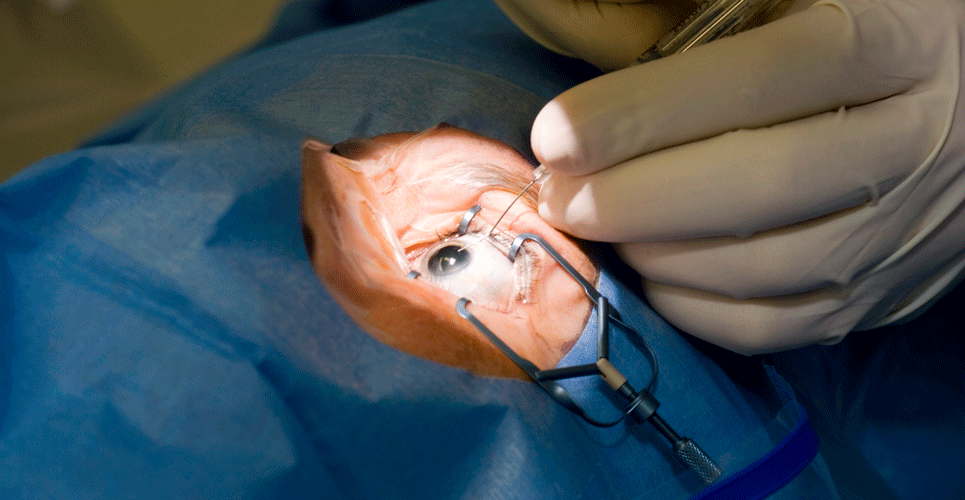
An RCT has found no reduction in the need for cataract surgery over a 5-year period among individuals given high-dose vitamin D
The level of cataract surgery performed among older adults did not reduce after 5-years of routinely supplementing with high-dose vitamin D compared to placebo according to the findings of a randomised trial by Australian researchers.
A cataract is a clouding or opacification of the normally clear lens of the eye or its capsule that obscures the passage of light through the lens to the retina. It is an extremely common condition with an estimated 95 million people worldwide affected and represents the leading cause of blindness in middle-income and low-income countries. Cataract surgery is a relatively common medical procedure involving the extraction of the lens from an eye and data show that the procedure was conducted round 4.5 million times in 2016 across the EU Member States. The potential role of vitamin D in the development of a cataract has been suggested due to the presence of its receptors within the eye and research on how expression of the receptor plays a significant role during retinal vascular development, especially during maturation of retinal vasculature. Additionally, observational data has shown that the risk of age-related cataract is reduced in men with higher serum 25-hydroxyvitamin D levels after adjusting for potential confounding factors. Nevertheless, this has not been a consistent finding with other study concluding that there does not appear to be a role for vitamin D in cataractogenesis among men. But as the currently available evidence is largely observational in nature, the Australian team undertook a randomised, controlled trial to determine if long-term supplementation with high-dose vitamin D might reduce the incidence of cataracts using the need for cataract surgery as a surrogate marker.
The Australian team used data generated from the D-Health trial, which enrolled adults aged between 60 and 79 years of age and which was designed to examine the effect of high-dose vitamin D (60,000 IU per month) on all-cause mortality. However, participant data collected included demographics and existing health conditions although baseline ophthalmic examinations were not included. The researchers set the primary outcome as the need for cataract surgery and although vitamin D levels were not measured in all participants, the researchers developed a model to predict baseline levels using data collected from a random sample of the participants.
Cataract surgery and vitamin D levels
A total of 19,925 individuals with a mean age of 69.3 years (46% female) were included and randomised to vitamin D (9941) or matching placebo and were followed for a median of 5 years.
A total of 3668 (18.4%) of the entire cohort underwent cataract surgery during follow-up and the rate was similar between the two groups (Hazard Ratio, HR = 1.02, 95% CI 0.95 – 1.09). In subgroup analysis, the incidence of cataract was higher among women (HR = 1.22, 95% CI 1.13 – 1.29) and in those aged over 75 years compared to ages 60 – 64 (HR = 3.53). There was also no difference between individuals with estimated vitamin D levels predicted to be either greater than or less than 50 nmol/L.
The authors concluded that there was no evidence to support the routine use of vitamin D in older adults as a strategy to reduce the need for cataract surgery.
Citation
Rahman ST et al. Vitamin D Supplementation and the Incidence of Cataract Surgery in Older Australian Adults Ophthalmology 2022