In July 2016, the UK Scientific Advisory Committee on Nutrition(SACN) recommended that to protect bone and muscle health, everyone should take a daily dose of 10 micrograms (equivalent to 400 IU) of vitamin D.
Indeed, over the years, various studies have shown a benefit from vitamin D supplementation and a reduction in bone fractures, particularly when combined with calcium for the prevention of osteoporotic fractures.
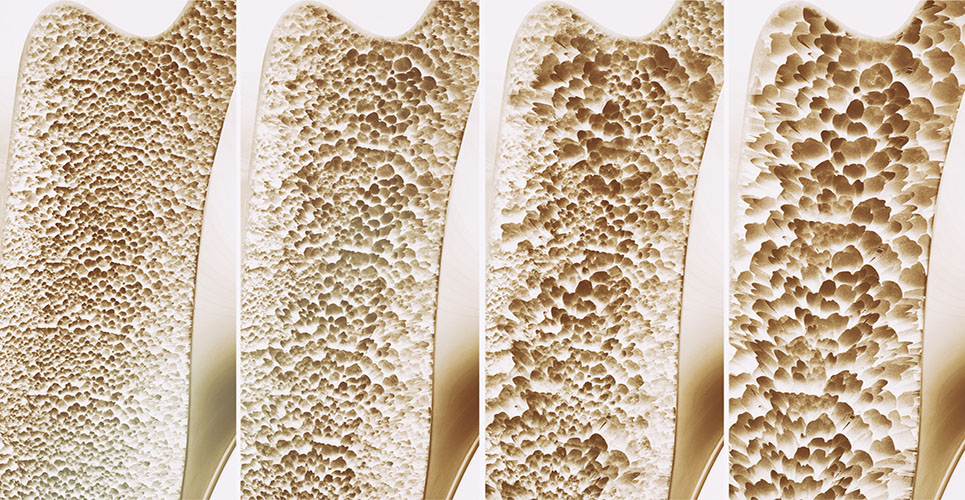
Vitamin D promotes the absorption of calcium in the intestines and helps maintain adequate levels of calcium and phosphorus, thus enabling normal bone mineralisation. Lack of vitamin D leads to greater bone resorption, bone loss and even loss of muscle function.
It is a fat soluble vitamin that is not widely present in foods (exceptions include oily fish, such as salmon, liver, cheese and egg yolks) and our major source is from the action of sunlight on the skin. However, many foods such as margarine, some breakfast cereals, infant formula milks and yoghurts are fortified with vitamin D to ensure that we meet the dietary recommendations.
Despite the importance of the vitamin, surveys suggest that low levels of vitamin D are present in nearly a quarter of patients aged 19-64 years and a fifth of those over 65 years of age.
However, one of the difficulties to trying to evaluate the effects of vitamin D is the lack of reliable evidence and no consensus as to what is meant by vitamin D deficiency. Normally, levels of 25-hydroxyvitamin D (25(OH)D), which is the major circulating metabolite of vitamin D, are used as a marker of vitamin D levels in the blood. It has been suggested that levels of 25(OH)D less than 30 nmol/litre represents a deficiency but also that 30-50 nmol/litre may be inadequate for some people. Levels greater than 50 nmol/litre are thought to be sufficient for most people.
While traditionally lack of vitamin D was thought to prevent rickets in children and osteomalacia (which is essentially ‘adult rickets’), the SACN report noted how it was not possible to determine whether rickets was due to a lack of vitamin D alone or both vitamin D and calcium.
But how robust is the evidence that vitamin D really does improve bone health and reduce the risk of fractures? In recent years, several studies have cast a doubt on the importance of supplementation. A recent Cochrane systematic review in 2014 concluded that ‘vitamin D alone is unlikely to prevent fractures in the doses and formulations tested so far in older people’.
A more recent randomised trial in patients aged over 70 with normal levels of 25-(OH)D, found that doses of vitamin D up to 48,000 IU per day for 12 months did not improve bone mineral density levels. In 2018, a comprehensive analysis of 81 randomised trials involving over 53,000 patients, found that vitamin D supplementation did not prevent fractures of falls or have important effects on bone density.
In more than half of the studies, patients had 25-(OH)D levels below 50 nmol/litre but in only 6% of trials were levels below 25 nmol/litre. A criticism of this analysis was that trials in which vitamin D were combined with calcium were excluded. However, a systemic review of increased calcium intake suggests that it does not help prevent fractures, even when combined with vitamin D.
This emerging evidence casts doubt on the value of supplementing with vitamin D as a strategy to improve bone health. Consequently, should pharmacists no longer recommend either calcium or vitamin D supplements for their elderly patients?
Although the SACN report indicated that the evidence for vitamin D in the prevention of fractures and falls was mixed and insufficient to draw any firm conclusions, it also noted that up to a quarter of those aged over 65 years and nearly 40% of institutionalised adults have 25-(OH)D levels below 25 nmol/litre.
Given that patients who are vitamin D deficient – which includes a large proportion of the elderly – have the most to gain from supplements, it would seem sensible to continue to reinforce the SACN advise that patients take a 10 microgram supplement of vitamin D at least until there is any change in the official advice.