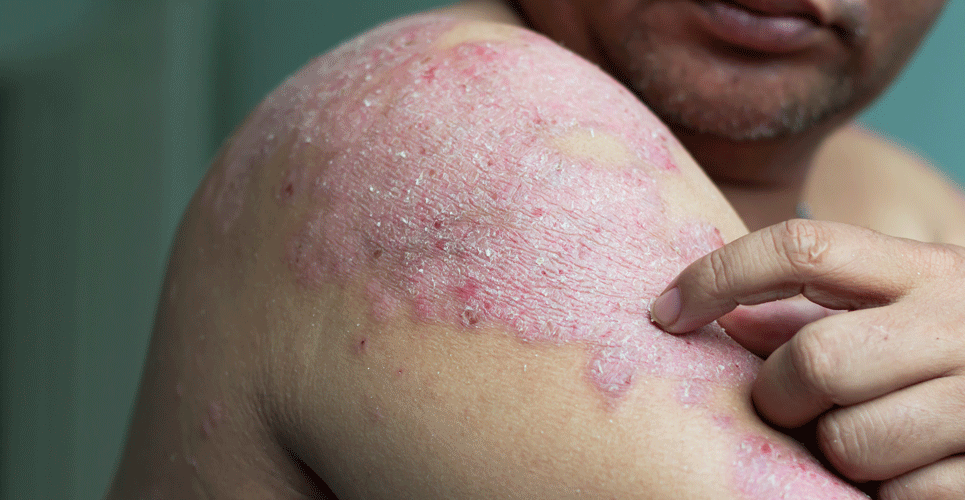
Tapinarof cream was found to be effective in two phase III, randomised placebo trials for patients with mild-to-moderate plaque psoriasis
Topical therapy with tapinarof 1% cream is effective for patients with mild-to-moderate plaque psoriasis when used over a 12 week period according to researchers from the Icahn School of Medicine at Mount Sinai, New York, US.
Psoriasis is defined as a common, chronic, recurrent, immune-mediated disease of the skin and joints and which affects around 125 million people worldwide that equates to between 2 and 3% of the population. Although patients with severe psoriasis can be managed with biologics, fortunately, the majority have mild-to-moderate psoriasis which can be adequately controlled with topical therapy, however, adherence to topical therapy is often suboptimal.
Tapinarof (TP) is a novel, non-steroidal, topical aryl hydrocarbon receptor-modulating agent and its mode of action is due to specific binding and activation of AhR, a ligand-dependent transcription factor, leading to the down-regulation of pro-inflammatory cytokines, including interleukin 17, and regulation of skin barrier protein expression to promote skin barrier normalisation.
In the present analysis, the authors combined the results obtained in two identical, randomised, double-blind, phase III trials, PSOARING 1 and PSOARING 2 which assessed TP 1% cream in adult patients (aged 18 years and over) with mild to moderate plaque psoriasis. Patients were randomised 2:1 (TP: placebo) and disease severity was assessed using the Physician’s Global Assessment (PGA) score which ranged from 0 (clear) to 4 (severe). The treatments were applied once daily and the primary efficacy endpoint was a PGA response, defined as a PGA score of 0 (clear) or 1 (almost clear) and a decrease from baseline of at least 2 points on the PGA scale. The main secondary outcome was the proportion of patients achieving a PASI 75 (which represents a 75% reduction in disease severity) and both assessments were made at week 12. The main patient reported outcome was a change of at least 4 points in the Peak Pruritus Numeric Rating Scale (PP-NRS) based on an 11-point (where 0 is no itch and 11 is the worst imaginable itch).
Findings
A total of 510 and 515 patients were enrolled and randomised to TP or placebo. In both trials, participants had a mean age of approximately 49 years and the proportion of male patients ranged from 50.6 to 62.6%. At entry, between 79.7 and 84% of participants had a PGA score of 3 (i.e., moderate disease severity) and a PP-NRS score of approximately 5.7.
The primary end point was achieved by 35.4% and 40.2% of patients in the tapinarof groups in both trials compared to 6% and 6.3% in those assigned to placebo (p < 0.001 for both trials). In addition, 36.1% and 47.6% of the intervention groups achieved a PASI 75 compared to 10.2% and 6.9% in the placebo groups (p < 0.001 for both trials). However, while reductions in PP-NRS scores were numerically higher in both tapinarof groups this difference was not reported as statistically significant.
The authors reported that overall, adverse events in the tapinarof group were higher 50.3% vs 22.4% in PSORING 1 and a similar proportion was seen in the second trial. The most frequent adverse events were folliculitis, nasopharyngitis, contact dermatitis and headache, all of which were more common with tapinarof.
They concluded that while tapinarof was more effective than placebo, larger and longer trials were required to evaluate its efficacy compared to existing topical psoriasis treatments.
Citation
Lebwohl MG et al. Phase 3 Trials of Tapinarof Cream for Plaque Psoriasis N Engl J Med 2021